Have you ever asked yourself why you do what you do?
I spent the first year after my residency working as an independent contractor in corporate dentistry. It was a tremendous opportunity being able to learn the business of orthodontics without the responsibility of ownership. As time went on, though, I began to realize the value of team culture and the key factors that influence new patient conversion. If I were to achieve my ultimate goals, I needed to take on the high risk of building an orthodontic practice from scratch. In 2013, I opened my office and began to experience what I consider to be the rewarding result of one of the most significant decisions I have ever made.
Author and motivational speaker Simon Sinek explains, “People don’t buy what you do, they buy why you do it.” As orthodontists, we all straighten teeth—that’s what we do. Our artistic signature, our brand, our unique practice fingerprint—our purpose, cause or belief—are the whys of what we do.
When our “why” goes fuzzy, it becomes difficult to maintain growth and inspire our teams and patients. We can apply the “why” approach not only to our office culture but also to our diagnosis and treatment planning. With each new patient case, we have the opportunity to reflect on our treatment plan and ask ourselves why we’ve decided to treat the patient the way we have, then confidently convey that to them. I’ll use a recent case as an example.
Diagnosis
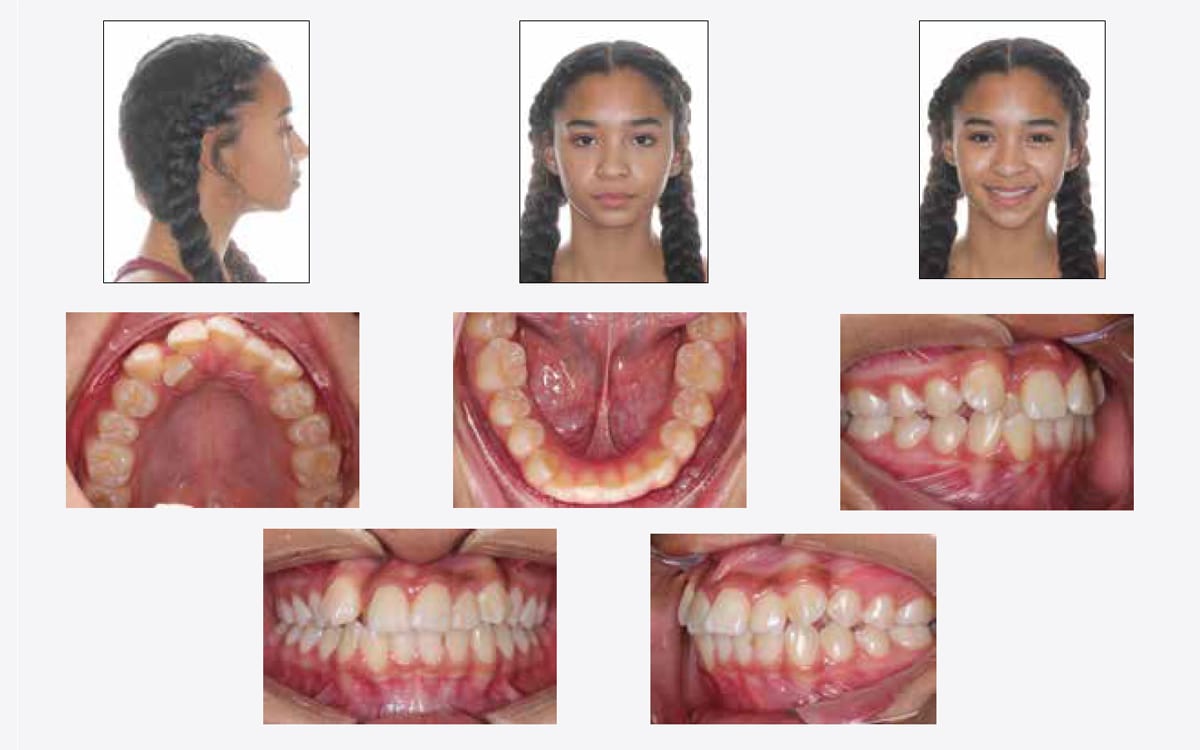
Meet Jada, a 14-year-old patient seeking to improve her smile and appearance through orthodontic treatment. She takes to the internet, searches for the nearest orthodontists, then verifies her choices on Instagram before asking her mom to call your office to schedule an appointment. You’re one of several orthodontists they’ll visit over the following weeks. At the initial exam, Jada seems a little fearful about what your treatment is going to entail and how it’s going to impact her social life. She tells you she doesn’t like how her teeth overlap in the front and how it appears as if she’s “missing a tooth.”
Your diagnosis likely includes a balanced facial profile with minimal incisal display on smiling, Class II malocclusion, transverse deficiency, anterior crossbite, severe crowding of the maxillary dentition, and moderate crowding of the mandibular dentition. What’s your treatment plan?
Buying your “why”
Jada’s diagnostics at initial presentation are likely not too different from what you see daily, and might even be considered routine in your office. However routine her case may be, she’s found your treatment plan to be unique among the several orthodontists in the area, which leaves her confused: She presented with the same set of problems at each office, so why is she hearing different treatment plans, lengths of treatment and costs?
She’s doing her best to sort through the plans, which include extractions, rapid palatal expansion, interproximal reduction, headgear and non-extraction therapy. There’s no single “right” way to treat her situation; there are just different ways among many acceptable treatment routes.
Jada says she has no reason to doubt that each orthodontist she visited has the skill and ability to straighten her teeth, simply because that’s what orthodontists do. In the end, however, she bought my “why”—not so much because of the treatment plan, per se, but because she could see how I’d be able to do something for her in terms of comfortable treatment (no rapid palatal expander) and maintaining her balanced facial aesthetics (no extractions).
Jada’s journey
When I see cases like this one, I ask myself, “Why is there crowding?” Is it that the patient truly has small jaws that can’t accommodate the teeth? I say usually not; there are often things that happen developmentally that push things in the wrong direction. In Jada’s case, perhaps her upper right primary tooth hung in too long, which didn’t allow adequate space for the eruption of the adult teeth. With this happening, her teeth started slipping forward and she ended up in crossbite.
If this is the case, why aggravate the problem by extracting teeth that further pushes them in the wrong direction—why not reverse the process? Non-extraction therapy using the light-force mechanics of the Damon philosophy is a restorative approach to orthodontics that’s respectful of the periodontal ligament and comfortable for patients. Of course, with adults it’s a little different situation, but the system works essentially the same way.
Treatment planning for long-term facial aesthetics usually means making a decision that a case can be treated non-extraction. This patient exhibited severe crowding in the upper arch, along with an almost completely blocked-out upper right lateral incisor. I’ve worked with the Damon system long enough to understand its capabilities and had confidence that with this passive system, using the proper mechanics, we could get a beautiful finish without an expander or extractions.
Treatment starts with proper bracket positioning for smile-arc protection or enhancement and disarticulation at bonding. Disarticulation disengages the arches and allows the light-force wires of this passive bracket system to operate more freely. It really comes down to the lateral development you get with this system, keeping the forces light. Once the lateral development is achieved, there will be room for resolving the crowding non-extraction.
Treatment plan and case progression
We offered Jada a treatment plan that didn’t require removing permanent teeth or the need for a rapid palatal expander. We selected the newest addition to the Damon appliance system, the Damon Q2 bracket in standard torque. (The variable torque DQ2 brackets had not yet been released.) The key to this system case management is to begin with light wires and disarticulation. Light wires stimulate the cells within the periodontal ligament and avoid crushing the blood vessels within. As with most of these cases, we began with a 0.014 nickel titanium (NiTi) wire engaged in each arch 6–6. At two months, the UR2 was bonded, a NiTi open-coil spring was placed, and an elastic thread was activated from the UR2 to the spring. The thread offers just enough activation to maintain proper arch form and allow the spring to express lateral forces.
Treatment progressed through the archwire sequence (all NiTi wires) to 0.018, 0.014×0.025 and 0.018×0.025 to gain the majority of the space required through lateral expansion. Keep in mind that the same spring and thread mechanics were maintained throughout this sequence with very light activation. The majority of the space required to engage the UR2 was through posterior arch development, not from the open-coil spring.
At about 12 months, we were able to drop back to a 0.014 NiTi wire to engage the UR2, progressing through the archwire sequence once again (from 0.014 to 0.018 to 0.014×0.025) before finally moving into the 0.019×0.025 finishing wire.
Interproximal reduction (IPR) was performed U3–3 to reduce unwanted black triangle spaces, common with severe crowding and anterior crossbite cases. Performing IPR is an essential component to finishing with broad flat contacts, minimizing or eliminating distracting black triangles. Class II elastics were utilized to address the A/P discrepancy. For space closure, we run elastic closing chain 7–7 for one visit at most and always under the wire.
Transverse arch development through the use of Damon light-force mechanics allows the expression of anterior crowding into the space gained in the posterior. Disarticulation, posterior arch development, and controlling the mechanics were the focus of this case. Moreover, the rotational control built into the DQ2 bracket and its refined slot tolerances mean you can finish with excellent control.
Results
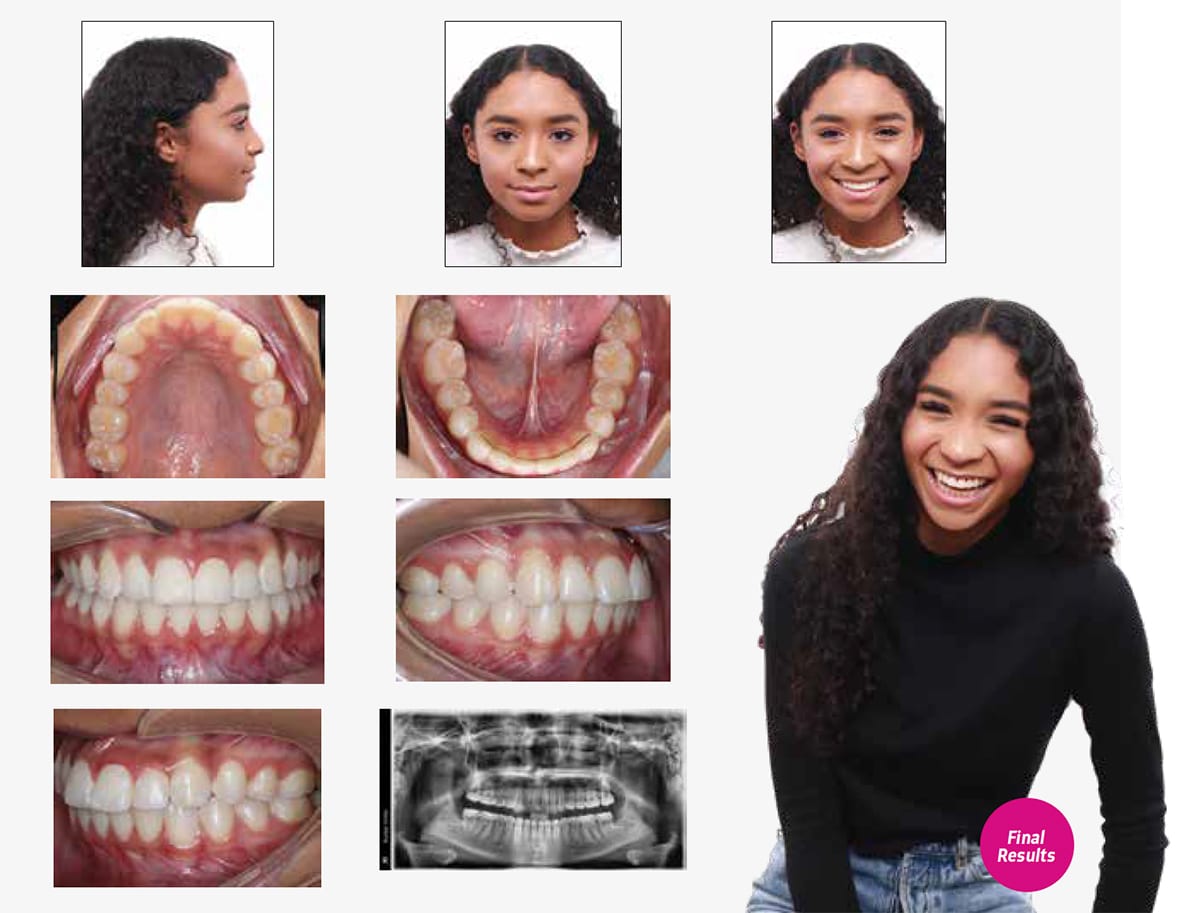
This case resolved to a more than satisfactory finish in 18 months to a Class I occlusion. The case is retained with a bonded retainer L3–3 with removable U/L clear retainers. The transverse development was key to resolving her maxillary anterior crossbite and severe crowding. Her balanced pretreatment facial profile, which would have been marred had extraction therapy been employed, was beautifully maintained.
Conclusion
The Q2 bracket has several key advantages that this case exemplifies. The most important of these advantages is its means for transverse development that allows such crowded cases to be treated non-extraction with no expansion devices. This bracket, combined with Damon system mechanics, created the critical space necessary to achieve this beautiful full-tooth smile while negating the adverse side effects of anterior flaring.
Schedule Your Free Consultation
NOTE: The author, Dr. Jonathan Rucker, is a certified specialist in orthodontics (Orthodontist). His private orthodontic practice, Rucker Orthodontics, is located in Temecula, California. He received a Bachelor of Science degree at Brigham Young University, his Doctor of Dental Surgery (DDS) from the Medical College of Virginia, and his orthodontic specialty training at Saint Louis University Center for Advanced Dental Education. He is a certified Damon Braces provider and a preferred Invisalign specialist. He offers the most advanced techniques available in modern orthodontic treatment to ensure his patients achieve their best possible results.